- Denise Lane; EAMP, LAc.1010 S. 3rd St.
(Dayton General Hospital)
Dayton, WA 99328509-382-3202
Physical Therapy Dept. Clinic Hours:
Tuesday-Thursday11am - 5pmSaturday12pm - 5pm
- Sign up to receive news and updates and get my free report:“The Top 10 Reasons to Try Acupuncture”

Follow Us!
-
- Testimonials
I had a great first visit today. Excellent service, I feel less stressed, and pain lightened up. Looking forward to my next visit.
J.V., Dayton, WA.
Two years ago I took a tumble off a horse and landed on my back.
For the first week after the accident, I could not walk upright and my entire back was in pain due to injury and sore muscles. Spasms and shooting pain would hit me any time of the day or night. Ice, heat and pain relievers were not improving my situation at all.
I finally sought treatment from Denise. For a week she did acupuncture,
... Read more »Some could call me a bit of a skeptic and acupuncture was at the top of my list – enter Denise!
I have become so dis-enchanted with traditional methods to my issues and the time I’ve spent with Denise has rocked my world!!! Acupuncture is helping me cope with my stress, the pain in my knee is subsiding and my lifelong abdominal issues are getting some much needed attention.
One appointment with Denise and I feel like
... Read more »I’ve had acupuncture from a number of therapists over the years and Denise ranks as one of the best. She has treated me for headaches, neck pain and constipation. All my symptoms have shown great improvement! I can’t recommend her highly enough.
G.R.; Pomeroy, WA.
I’ve known Denise for a few years now and have received acupuncture treatment from her for lower back pain and stress. It gave me instant relief. Denise is great at what she does and has been a wonderful resource for me to have.
G.W.H., Portland, Or.
I went to get acupuncture from Denise Lane for two problems, gout and stress. I am doing well enough that I have not had to return for follow up treatments for three months. She is very caring and straight forward.
–G., Waitsburg, Wa.
-
Latest Articles:
- • The Best Ways to Protect Your Skin from the Sun This Summer •
- • Savoring Summer with Recipes Using the Best Summer Ingredients •
- • Top 5 Best Staycation Ideas for Summer •
Research Articles
Research: Biochemical Reaction Shows How Acupuncture Works
Acupuncture Pain Killing Mystery Revealed
June 28, 2014
HealthCMI
Researchers have discovered that acupuncture causes a special biochemical reaction that reduces inflammation and muscle pain. The study, published in Molecular Neurobiology, investigated the effects of needling one acupuncture point on the leg. The research team measured a remarkable effect. Acupuncture point SP6, Sanyinjiao, is depicted in this image. Manual acupuncture stimulation downregulated M1 macrophages (pro-inflammatory cells) and upregulated M2 macrophages (anti-inflammatory cells). As a result, acupuncture reduced pain and swelling.
This neurobiological acupuncture continuing education study solves a great mystery, how does acupuncture work? The secret is in 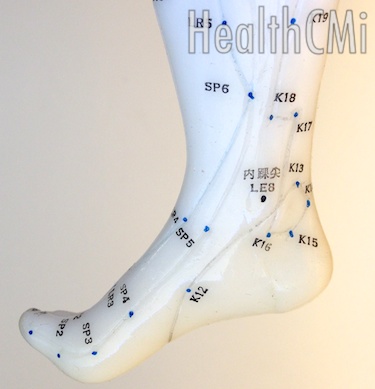 the biochemistry. M2 macrophages are an important source of IL-10 (interleukin-10), an anti-inflammatory cytokine that plays an important role in immune responses. Cytokines are proteins released by cells that regulate reactions between cells. Manual acupuncture successfully downregulates M1 macrophages and upregulates M2 macrophages thereby promoting the release of greater IL-10 concentrations. As a result of IL-10 release, pain and inflammation significantly reduce.
the biochemistry. M2 macrophages are an important source of IL-10 (interleukin-10), an anti-inflammatory cytokine that plays an important role in immune responses. Cytokines are proteins released by cells that regulate reactions between cells. Manual acupuncture successfully downregulates M1 macrophages and upregulates M2 macrophages thereby promoting the release of greater IL-10 concentrations. As a result of IL-10 release, pain and inflammation significantly reduce.
This study measured responses in muscle tissues and confirmed that M1 to M2 macrophage phenotype switching is triggered by acupuncture stimulation. Acupuncture literally flips a switch wherein initial inflammatory responses are reduced and the secondary healing responses are promoted. M1 macrophage downregulation and M2 macrophage upregulation triggered by acupuncture was positively associated with reductions in muscle pain and inflammation.
The researchers tested the biochemical process by adding an IL-10 blocking agent in the laboratory experiment. When IL-10 was chemically blocked, acupuncture did not reduce pain and swelling. However, when no blocking agent was applied, acupuncture successfully reduced both pain and swelling. The M2 macrophage upregulation by manual acupuncture successfully created a greater source of IL-10. The researchers note, “These findings provide new evidence that MA (manual acupuncture) produces a phenotypic switch in macrophages and increases IL-10 concentrations in muscle to reduce pain and inflammation.”
Macrophages are required by the body to resolve muscle injury. During injury, M1 macrophages are produced and release inflammatory biochemicals including pro-inflammatory cytokines. M2 macrophages have anti-inflammatory properties and promote the release of interleukin-10. An injury process features an initial inflammatory stage wherein M1 pro-inflammatory macrophages are upregulated. A secondary recovery phase wherein M2 anti-inflammatory macrophages are upregulated helps to promote healing and repair. Manual acupuncture successfully triggered the phenotype switch wherein the M1 macrophages were downregulated and M1 macrophages were upregulated thereby allowing increased IL-10, reductions in pain and decreased swelling.
Acupuncture continuing education in the form of basic research and clinical medicine has helped to measure positive patient outcomes and the biochemical mechanisms by which acupuncture exerts its beneficial medical effects. This latest study helps to unlock one of the greatest secrets of acupuncture, how does it stop pain? Now, scientists can quantifiably measure specific biochemical processes triggered by acupuncture and the resultant positive health outcomes.
Getting To The Point
The acupuncture point tested in this investigation was SP6 (Sanyinjiao, Three Yin Intersection). SP6 is located 3 cun directly above the tip of the medial malleolus, on the posterior border of the medial aspect of the tibia. According to Traditional Chinese Medicine (TCM) theory, SP6 strengthens the spleen, transforms dampness, spreads liver qi and benefits the kidneys. SP6 indicated for the treatment of abdominal pain & distention, diarrhea, dysmenorrhea, irregular menstruation, uterine bleeding, leukorrhea, prolapse of the uterus, sterility, difficult or delayed labor, nocturnal emissions, enuresis, dysuria, lower limb atrophy or motor impairment, lower limb hemiplegia, vertigo due to blood deficiency and insomnia. SP6 is the meeting point of the three lower yin meridians: spleen, liver and kidney. A globe and DNA are represented here.
About HealthCMi: The Healthcare Medicine Institute (HealthCMi) publishes news and research on acupuncture, herbal medicine and traditional medicine. HealthCMi provides acupuncture CEU and NCCAOM PDA online courses to licensed acupuncturists for acupuncture continuing education credit. To submit an article for publication consideration, visit www.healthcmi.com and click on the contact us link.
References:
da Silva, Morgana D., Franciane Bobinski, Karina L. Sato, Sandra J. Kolker, Kathleen A. Sluka, and Adair RS Santos. “IL-10 Cytokine Released from M2 Macrophages Is Crucial for Analgesic and Anti-inflammatory Effects of Acupuncture in a Model of Inflammatory Muscle Pain.” Molecular Neurobiology (2014): 1-13.
Rafael Torres-Rosas, Ghassan Yehia, Geber Peña, Priya Mishra, Maria del Rocio Thompson-Bonilla, Mario Adán Moreno-Eutimio, Lourdes Andrea Arriaga-Pizano, Armando Isibasi, Luis Ulloa. Dopamine mediates vagal modulation of the immune system by electroacupuncture. Nature Medicine, 2014; DOI: 10.1038/nm.3479.
Wang, Ying, Rebekka Gehringer, Shaaban A. Mousa, Dagmar Hackel, Alexander Brack, and Heike L. Rittner. “CXCL10 Controls Inflammatory Pain via Opioid Peptide-Containing Macrophages in Electroacupuncture.” PloS one 9, no. 4 (2014): e94696.
– See more at: http://www.healthcmi.com/Acupuncture-Continuing-Education-News/1336-acupuncture-pain-killing-mystery-revealed#sthash.oduvXBB3.dpuf
Acupuncture Beats Drugs For Shingles Nerve Pain
Acupuncture Beats Drugs For Shingles Nerve Pain
Acupuncture combined with moxibustion was determined more effective than the drug gabapentin for the treatment of shingles, herpes zoster. New research compared the effects of acupuncture followed by local moxibustion against a group that received gabapentin and sham acupuncture. The true acupuncture group had an effective rate of 94% and the drug group had an effective rate of 86%. Acupoints for shingles. Gabapentin (neurontin) is a pharmaceutical medication often used to treat nerve pain, especially in cases nerve pain due to shingles (post-herpetic neuralgia). True acupuncture was applied to Ashi points. Sham acupuncture is a form of simulated acupuncture used to help establish controls in clinical investigations and assists in ruling out the placebo effect. In this study, sham non-acupuncture points were needled in the distal region of the herpetic lesions. This type of sham control has received recent criticism by researchers in that sham needling may provide medical benefits thereby skewing data towards underestimating the healing powers of true acupuncture. Moxibustion involves burning herbs, usually Ai Ye (mugwort), near the skin to provide penetrating warmth. Moxibustion is often combined with acupuncture by licensed acupuncturists in clinical settings. In this study, moxibustion (moxa) was applied for 15 minutes in the region of the lesions. The treatment of shingles has historically been treated by acupuncture within the Traditional Chinese Medicine (TCM) system for well over 1,000 years. This new research confirms the efficacy of acupuncture for the treatment of nerve pain related to the sequela of shingles. The team estimated the cost of care for both groups and determined that acupuncture is both effective and cost-effective for the treatment of nerve pain due to shingles. Doll with acupoints. TCM The historical treatment of shingles with acupuncture often involves, according to TCM principles, the treatment of endogenous damp heat. A Zang-Fu diagnosis may confirm excess liver and gallbladder fire and exogenous toxins. Treatment may involve acupuncture points LI11 (Quchi), SP10 (Xuehai), UB40 (Weizhong), GB34 (Yanglingquan) and LV3 (Taichong). According to TCM principles, this combination of acupuncture points dispels wind, clears heat toxins, clears heat in the blood and clears liver and gallbladder damp heat.
Reference: Huang, S. X., M. Mao, J. J. Pu, Y. H. Chen, L. Deng, H. Zhao, M. J. Geng et al. “Clinical research on fire filiform needle combined with mild moxibustion for postherpetic neuralgia.” Zhongguo zhen jiu [Chinese acupuncture & moxibustion] 34, no. 3 (2014): 225. – See more at: http://www.healthcmi.com/Acupuncture-Continuing-Education-News/1314-acupuncture-beats-drugs-for-shingles-nerve-pain#sthash.rHpSfuXa.dpuf
Mental Well-being and Acupuncture
Blue Valley Acupuncture Clinic-Located in Dayton, WA.-serving greater Walla Walla area & nearby towns.
Mental Well-being and Acupuncture
Article attributed to HealthCMI
One of the most rewarding aspects of being a licensed acupuncturist is to deliver fast clinical results that directly improves the life of the patient. Acupuncture for the treatment of panic attacks is one of the more dramatic treatment protocols because of the immediate impact it has on patients’ lives. Often, from the time of the very first acupuncture treatment, the patient has a decrease in the frequency, intensity and duration of panic attacks. As the process continues, patients gain a greater sense of well-being, centeredness, self-confidence and control over their lives.
I remember treating a Vietnam veteran about ten years ago. Decades after his extreme combat experiences, he had never slept more than two complete hours consecutively. The stress, exhaustion and mental restlessness had withered this man to a shell of what he once was. Psychologically, he had made peace wit his past. Physiologically, however, his body and brain chemistry had suffered from post traumatic stress syndrome (PTSD) and he was unable to fully recover from the impact of his experiences.
After the first acupuncture treatment he was able to sleep up to about four hours per night. After a few weeks of acupuncture, his sleep pattern normalized. He no longer experienced panic attacks and no longer woke up covered in sweat from nightmares. He came in to my office for routine checkups until he felt fully recovered. It was incredible to see his face change. The stress fell from his eyes and cheeks. His complexion returned. His wooden exterior softened into that of a happy man. Eventually, he fell in love and got married.
Most panic attack patients at my clinic tend to be hard working individuals with very busy schedules. Everyday stresses in the workplace combined with family and relationship struggles tend to build up in the system until the psyche breaks. Combine some of the aforementioned issues with lack of time for reflection and rest, financial struggles and maybe a lack of community support and the average person may see the emergence of panic attacks. Here, Liver Qi Stagnation has the opportunity to turn into Liver Fire. It may also create a cycle of Liver Qi depression with either Yang Uprising or excess Fire. Naturally, the Heart Shen is poorly nourished as the Liver Yin is depleted. The Qi, Blood, Yin and Yang may be depleted and the consequent stagnation and lack of Yin essence may also create excess Fire. In some cases, Heat in the Blood may develop along with its associated bleeding disorders. Abnormal uterine bleeding and sensory organ disorders are not uncommon in these circumstances.
It’s amazing what a simple release can do for one’s spirit. In some instances, acupuncture is akin to releasing pressurized steam from a tea kettle. Patients with extremely high stress loads may spurt a high pressure mist of blood that emanates from Yin Tang when the needle is removed. It reminds me of an aerosol spray. I usually let my patients know they can expect significant clinical results and a good night’s sleep if I see this release, especially when combined with a release of blood from ear Shenmen when the needle is removed. Naturally, an acupuncturist can analyse the color of the blood released from ear Shenmen to make a more detailed diagnosis.
Common body acupuncture points for the treatment of panic attacks are P7, P6, TB5, HT7, LI11, Sishencong, Yintang, LR3, DU20 and ST44. Nourishing points for patients with panic attacks often include ST36, SP6, K3, and K7. Auricular points vary dependent upon the system used, however, ear Liver, Kidney, Heart, Brain, Sympathetic and Shenmen are common amoung the standard auricular points. In patients prone to depression, using DU24 with a triple side-by-side technique combined with the Chouqi technique simultaneouly on all three points helps to direct the healthy energy upwards while releasing stagnation from the mind and Shen. In all, an acupuncturist simply needs to stick with a classical differential diagnosis to ensure that the upward and descending movement Qi becomes balanced. Some will need strong tonification while many will need better invigoration and circulation of Qi and Blood.
Heavy sedation acupuncture points are often necessary in acute cases wherein the patient may have difficulty in maintaining sanity or composure. This is more common in patients with schizophrenia. Often, acupuncture can reduce a multitude of voices inside the head of the patient to a singular identity during the treatment. I can’t help but have compassion for these individuals. They often feel like they are living in a crowded room of voices and cannot discern their own. Although acupuncture brings significant and immediate results, the acupuncture is useless without tremendous family or community support. For patients suffering from schizophrenia, regularity and discipline are difficult. They fall from their medication regimes and acupuncture treatment schedules. They often engage in behaviors such as staying out late and losing sleep combined with a poor diet. It’s a big job to help these people. Resolving panic attacks for the average patient is straightforward and rapid, however, for patients with schizophrenia this process may be ineffective due to lack of follow through on the patient’s behalf.
Patients suffering from depression and diabetes are another challenge. In both cases, they will respond more slowly to treatment for most disorders. If a patient suffers from both disorders simultaneously, it presents significant clinical challenges. Results will probably come about more slowly. Also, significant attention must be devoted to restoring the patient’s insulin-glucagon pathway. Mental instability due to blood glucose level fluctuations exacerbates the recovery process. Even so, patients with depression and diabetes will usually see resolution of their panic attacks in a timely fashion with the disciplined application of acupuncture care.
– See more at: http://www.healthcmi.com/Acupuncture-Blog/723-panicattacksshenmen#sthash.iLatrww9.dpuf
NY TIMES ARTICLE-ACUPUNCTURE PAIN STUDY
BLUE VALLEY ACUPUNCTURE CLINIC-LOCATED IN DAYTON, WA.-SERVING GREATER WALLA WALLA, WA. AREA AND NEARBY TOWNS.
Acupuncture Provides True Pain Relief in Study
By ANAHAD O’CONNOR SEPTEMBER 11, 2012, 12:53 PM
 Acupuncture may be helpful in treating migraines, arthritis and chronic pain.
Acupuncture may be helpful in treating migraines, arthritis and chronic pain.
Gordon Welters for The New York Times
Acupuncture may be helpful in treating migraines, arthritis and chronic pain.
A new study of acupuncture — the most rigorous and detailed analysis of the treatment to date — found that it can ease migraines and arthritis and other forms of chronic pain.
The findings provide strong scientific support for an age-old therapy used by an estimated three million Americans each year. Though acupuncture has been studied for decades, the body of medical research on it has been mixed and mired to some extent by small and poor-quality studies. Financed by the National Institutes of Health and carried out over about half a decade, the new research was a detailed analysis of earlier research that involved data on nearly 18,000 patients.
The researchers, who published their results in Archives of Internal Medicine, found that acupuncture outperformed sham treatments and standard care when used by people suffering from osteoarthritis, migraines and chronic back, neck and shoulder pain.
“This has been a controversial subject for a long time,” said Dr. Andrew J. Vickers, attending research methodologist at Memorial Sloan-Kettering Cancer Center in New York and the lead author of the study. “But when you try to answer the question the right way, as we did, you get very clear answers.
“We think there’s firm evidence supporting acupuncture for the treatment of chronic pain.”
Acupuncture, which involves inserting needles at various places on the body to stimulate so-called acupoints, is among the most widely practiced forms of alternative medicine in the country and is offered by many hospitals. Most commonly the treatment is sought by adults looking for relief from chronic pain, though it is also used with growing frequency in children. According to government estimates, about 150,000 children in the United States underwent acupuncture in 2007.
But for all its popularity, questions about its efficacy have long been commonplace. Are those who swear by it experiencing true relief or the psychological balm of the placebo effect?
Dr. Vickers and a team of scientists from around the world — England, Germany, Sweden and elsewhere — sought an answer by pooling years of data. Rather than averaging the results or conclusions from years of previous studies, a common but less rigorous form of meta-analysis, Dr. Vickers and his colleagues first selected 29 randomized studies of acupuncture that they determined to be of high quality. Then they contacted the authors to obtain their raw data, which they scrutinized and pooled for further analysis. This helped them correct for statistical and methodological problems with the previous studies, allowing them to reach more precise and reliable conclusions about whether acupuncture actually works.
All told, the painstaking process took the team about six years. “Replicating pretty much every single number reported in dozens of papers is no quick or easy task,” Dr. Vickers said.
The meta-analysis included studies that compared acupuncture with usual care, like over-the-counter pain relievers and other standard medicines. It also included studies that used sham acupuncture treatments, in which needles were inserted only superficially, for example, or in which patients in control groups were treated with needles that covertly retracted into handles.
Ultimately, Dr. Vickers and his colleagues found that at the end of treatment, about half of the patients treated with true acupuncture reported improvements, compared with about 30 percent of patients who did not undergo it.
“There were 30 or 40 people from all over the world involved in this research, and as a whole the sense was that this was a clinically important effect size,” Dr. Vickers said. That is especially the case, he added, given that acupuncture “is relatively noninvasive and relatively safe.”
Has acupuncture worked for you? Join in the discussion.
Dr. Vickers said the results of the study suggest that people undergoing the treatment are getting more than just a psychological boost. “They’re not just getting some placebo effect,” he said. “It’s not some sort of strange healing ritual.”
In an accompanying editorial, Dr. Andrew L. Avins, a research scientist at Kaiser Permanente who focuses on musculoskeletal pain and preventive medicine, wrote that the relationship between conventional medical care “and the world of complementary and alternative medicine remains ambiguous.” But at least in the case of acupuncture, he wrote, the new study provides “robust evidence” that it provides “modest benefits over usual care for patients with diverse sources of chronic pain.”
SHARE
Acupuncture Effective for Low Back Pain-Serving Walla Walla, WA., Dayton Wa.
ACUPUNCTURE EFFECTIVE FOR CHRONIC LOW BACK PAIN
Blue Valley Acupuncture Clinic-Serving Walla Walla, WA., Dayton & nearby towns.
Article courtesy of HealthCMI
ON 29 APRIL 2014.
Researchers conclude that acupuncture is effective for the treatment of chronic low back pain. A randomized, controlled trial was performed at the Dongzhimen Hospital in Beijing, China with a group of 60 participants. Acupuncture effectively decreased patient pain levels and reduced days missed from work due to low back pain. Back Points
Another study of 236 patients published in the Journal of Musculoskeletal Pain concludes that acupuncture is effective for the treatment of low back pain. A total of 14 acupuncture treatments were administered over 4 weeks in this randomized trial. The researchers concluded that acupuncture has “beneficial and persistent effectiveness against CLBP (chronic lower back pain).”
Another study investigated the effects of distal acupuncture on low back pain. Distal acupuncture involves acupuncture point selections from areas that are not located in the affected region. For this study, a single acupuncture point, LI4 (Hegu), was chosen. A group of 187 patients with chronic low back pain received 18 treatments at LI4 over a 7 week period in this controlled clinical trial. The patients demonstrated significant relief from low back pain.
LI4 is located on the dorsum of the hand, between the 1st and 2nd metacarpal bones at the midpoint of the 2nd metacarpal bone, at the high point of the thenar eminence and distal to the transverse carpal ligament. In Traditional Chinese Medicine (TCM), acupuncture is applied to this point for the treatment of many pain related conditions including headaches, jaw pain, eye pain and toothaches. Nearby, another well known set of distal points on the hand, Yaotongxue, are often used by licensed acupuncturists for the relief of pain due to acute low back sprain.
Hegu, LI4
A large scale analysis of a multitude of studies finds acupuncture effective for the relief of low back pain. In a meta-analysis of 11 randomized-controlled trials, researchers note that “current evidence is encouraging in that acupuncture may be more effective than medication….” They note that, “Compared with nonsteroidal anti-inflammatory drugs, acupuncture may more effectively improve symptoms of acute LBP (lower back pain).” The study eliminated variables such as the placebo effect by using sham (simulated) acupuncture controls to ensure the validity of the data.
Another study finds acupuncture effective for the treatment of neck and lower back pain. The researchers concur with prior studies demonstrating that acupuncture is effective for pain relief and that acupuncture is sometimes more effective than NSAIDs (nonsteroidal anti-inflammatory drugs). Acupuncture was determined to be effective for both long and short-term pain relief of lumbar disc herniations and cervical disc related pain.
Cost-Effectiveness
A great deal of press has been given to the administration of healthcare within the USA. Concern over implementation of recent healthcare legislation such as the PPACA (The Patient Protection and Affordable Care Act, “Obamacare”) has received enormous news coverage. Other systems providing healthcare for all its citizens including those of Canada, the UK, Australia, Germany and France have also received attention as a result of the new USA basic standards in healthcare insurance established by the PPACA. Acupuncture research has focused on this aspect of the conversation and not only on clinical effectiveness.
Researchers in Calgary, Alberta investigated the cost-effectiveness of acupuncture for the treatment of low back pain. They discovered that acupuncture reduces the total of health services spending. A group of 201 acupuncture and 804 non-acupuncture low back pain patients were evaluated for the number of medical doctor visits required for the treatment of low back pain.
The mean age of the group was 48 years and 54% of those investigated were female. Results were tabulated as a comparison of the 1 year period prior to receiving acupuncture therapy versus the 1 year period after having had acupuncture therapy. The same period of time was evaluated for the 804 non-acupuncture patients in the control group.
Cost Effective Medicine
The acupuncture group saw doctors 49% less after having acupuncture. The non-acupuncture patients had a decrease of only 2%. The acupuncture patients total monetary cost of physician services decreased by 37%. The non-acupuncture patients had a 1% drop in cost. The researchers concluded that low back pain patients are less likely to visit medical practitioners for low back pain after having had acupuncture therapy thereby reducing overall health service expenses.
Multidisciplinary approaches have also been studied. A new study finds that acupuncture combined with massage is more effective for treating lumbar disc herniation (LDH) than coenzyme B12 injections combined with physiotherapy. Researchers randomly divided 60 patients into an acupuncture group and an injection group. The acupuncture group received acupuncture needling on myofascial pain related trigger points combined with massage. The injection group received coenzyme B12 injections combined with traction and heat therapy. The acupuncture group achieved an overall effective rate of 96.7% and the injection therapy group had an 80.0% effective rate.
Other very serious investigations found acupuncture effective for back pain related to cancer pain. Researchers conducted a randomized, placebo controlled study to investigate whether or not acupuncture reduces pain associated with pancreatic cancer. This type of cancer is often accompanied by severe abdominal or back pain. The researchers concluded that, “Electroacupuncture was an effective treatment for relieving pancreatic cancer pain.”
The acupuncture points used in the study were the Jiaji points from T8 to T12, bilaterally, for a total of 30 minutes of acupuncture needle retention time per office visit. Treatment frequency was once per day for a total of 3 days of care. The placebo control group showed little to no change in pain levels. The electroacupuncture group showed a significant reduction in pain intensity levels.
This is not an exhaustive list of all of the acupuncture research to be published in recent years. Acupuncture now has an established track record for the relief of low back pain. This is supported by clinical trials, laboratory experiments and meta-analyses. In addition, mounting evidence now finds acupuncture cost-effective for the treatment of low back pain. The slow and steady integration of acupuncture into conventional medical settings combined with acupuncture continuing education and research now brings acupuncture into the mainstream for the treatment of acute and chronic pain.
Fire Cupping
References:
Bahrami-Taghanaki, H., Y. Liu, H. Azizi, A. Khorsand, H. Esmaily, A. Bahrami, and Zhao B. Xiao. “A randomized, controlled trial of acupuncture for chronic low-back pain.” Alternative therapies in health and medicine 20, no. 3 (2014): 13.
Mingdong, Yun. Na, Xiong. Mingyang, Guo. Jun, Zhang. Defang, Liu. Yong, Luo. Lingling, Guo. Jiao, Yan. Acupuncture at the Back-Pain-Acupoints for Chronic Low Back Pain of Peacekeepers in Lebanon: A Randomized Controlled Trial. Journal of Musculoskeletal Pain. P 107-115, V 20.
Hegu Acupuncture for Chronic Low-Back Pain: A Randomized Controlled Trial. Mingdong Yun, Yongcong Shao, Yan Zhang, Sheng He, Na Xiong, Jun Zhang, Mingyang Guo, Defang Liu, Yong Luo, Lingling Guo, and Jiao Yan. The Journal of Alternative and Complementary Medicine. February 2012, 18(2): 130-136. doi:10.1089/acm.2010.0779.
Acupuncture for Acute Low Back Pain: A Systematic Review. Lee, Jun-Hwan KMD, PhD; Choi, Tae-Young PhD; Lee, Myeong Soo PhD; Lee, Hyejung KMD, PhD; Shin, Byung-Cheul KMD, PhD; Lee, Hyangsook KMD, PhD. Clinical Journal of Pain:. POST AUTHOR CORRECTIONS, 6 August 2012.
Effectiveness of Acupuncture with NSAID Medication in the Management of Acute Discogenic Radicular Pain: A Randomised, Controlled Trial. Beyazit Zencirci1, Kasim Zafer Yuksel, and Yakup Gumusalan. J Anesthe Clinic Res 2012, 3:3.
Deutsche Zeitschrift für Akupunktur. Volume 55, Issue 3, 2012, Pages 25–26. Reduced health resource use after acupuncture for low-back pain. S Moritza, MF Liub, B Rickhia, b, c, TJ Xua, P Paccagnana, H Quand. Participating institutions: Canadian Institute of Natural and Integrative Medicine, Calgary, Alberta, Canada. Alberta Health Services, Calgary, Alberta, Canada. University of Calgary, Calgary, Alberta, Canada.
Chen, Hao, Tang-Yi Liu, Le Kuai, Ji Zhu, Cai-Jun Wu, and Lu-Ming Liu. “Electroacupuncture treatment for pancreatic cancer pain: A randomized controlled trial.” Pancreatology (2013).
Ting Bao, Lixing Lao, Michelle Medeiros, Ruixin Zhang, Susan G. Dorsey, and Ashraf Badros. Medical Acupuncture. September 2012, 24(3): 181-187. doi:10.1089/acu.2011.0868. The University of Maryland School of Medicine, Baltimore, Maryland.
– See more at: http://www.healthcmi.com/Acupuncture-Continuing-Education-News/1301-new-acupuncture-relief-from-low-back-pain#sthash.W1Lbs3dI.dpuf
Acupuncture Synergizes Epilepsy Relief-New Finding
BLUE VALLEY ACUPUNCTURE CLINIC-WALLA WALLA, WA., DAYTON & NEARBY TOWNS
 Article contributed by HealthCMI Acupuncture effectively alleviates epilepsy, a nervous system disorder characterized by unregulated brain cell activity causing seizures. New research finds acupuncture combined with medications is more effective than using only medications as a therapy for epilepsy. The research project, conducted at the Ninth People’s Hospital of Henan, randomly divided 60 cases of epilepsy equally into a control group and an acupuncture group. The control group received only pharmaceutical medications. Epilepsy is treated with the DU, REN and Heart channels. The acupuncture group received both scalp acupuncture and body acupuncture in addition to pharmaceutical medications. The acupuncture group demonstrated significantly superior patient outcomes over the medication only control group. Drugs and Acupuncture The control group received oral administration of sodium valproate. This pharmaceutical medication is an anticonvulsant commonly used in the treatment of epilepsy, anorexia nervosa and bipolar disorder. Adverse affects associated with sodium valproate include fatigue, tremors, sedation and digestive disturbances. During pregnancy, this medication poses a very high risk for birth defects. Sodium valproate was administered twice daily with a dosage of 15-35 mg/kg for 30 days, comprising one course. The treatment lasted for three courses. The acupuncture group received needling in addition to the administration of sodium valproate. Scalp acupuncture needling was applied to the chest area, the epilepsy-control area and the chorea-tremor control area. Body style acupuncture was applied to Fengchi (GB 20), Baihui (DU 20), Sishencong (EX-HN1), Yintang (EX-HN3), Shuigou (DU 26), Neiguan (PC 6), Hegu (LI 4), Zusanli (ST 36), Fenglong (ST 40), Sanyinjiao (SP 6) and Taichong (LR 3). DU 26 is a vital acupoint in refreshing the brain. According to Traditional Chinese Medicine (TCM) principles, this acupuncture point clears the senses, calms the spirit and benefits the lumbar spine. DU 26 is indicated for both seizures and epilepsy. PC 6 is the Luo-connecting point of the Hand Jueyin channel. In TCM, PC 6 is used to calm the heart and spirit, regulate qi and suppress pain. PC 6 is indicated for the treatment of palpitations, chest pain, seizures and epilepsy, nausea, vomiting and heart beat issues. The lifting and thrusting needle technique was applied to DU 26, PC 6, EX-HN3, DU 20, EX-HN1 and LI 4. The reinforcing-reducing method was applied to other acupoints until the patient felt soreness and numbness consistent with the arrival of deqi. The needles were retained for 30 minutes and 10 days comprised one course of care. There was a 2 day break following each course. The treatment period was a total of 3 months. Following the completion of acupuncture therapy, a total of 12 acupuncture group patients showed no epilepsy related symptoms for at least 1 year. A total of 9 patients showed excellent improvements and 6 patients showed moderate improvements. The overall effective rate for the acupuncture group was 90.00% compared to 73.33% for the control group. Based on the positive clinical outcome, the research concludes that acupuncture combined with sodium valproate has a synergistic clinical effect leading to improved patient outcomes. AcuOffice TCM Theory Epilepsy is manifest in seizures, loss of consciousness, foaming of the mouth, headaches, dizziness, a stifling sensation in the chest, pallor, clenched jaw, incontinence of urine and feces, screams and/or staring of the eyes. According to TCM principles, epilepsy is an excess condition although it may arise from deficiencies in chronic cases. The onset of heredity related epilepsy is usually during early childhood. In TCM, epilepsy involves internal liver wind, liver qi stagnation and may also be exacerbated by dampness in the spleen and stomach, particularly due to irregular food intake. Fear and fright may trigger epilepsy. Fear disorders the qi and fright descends the qi thereby causing liver and kidney related internal wind due to deficiency. DU, REN, and Liver channel points are often selected for treatment during a seizure. The focus is to revive consciousness, dissolve phlegm, soothe the liver qi and to dispel the wind. Heart, Spleen and Kidney channel points are commonly selected following a seizure. The treatment principle is to soothe the spirit, nourish the heart and kidneys and to strengthen the spleen and stomach.
Article contributed by HealthCMI Acupuncture effectively alleviates epilepsy, a nervous system disorder characterized by unregulated brain cell activity causing seizures. New research finds acupuncture combined with medications is more effective than using only medications as a therapy for epilepsy. The research project, conducted at the Ninth People’s Hospital of Henan, randomly divided 60 cases of epilepsy equally into a control group and an acupuncture group. The control group received only pharmaceutical medications. Epilepsy is treated with the DU, REN and Heart channels. The acupuncture group received both scalp acupuncture and body acupuncture in addition to pharmaceutical medications. The acupuncture group demonstrated significantly superior patient outcomes over the medication only control group. Drugs and Acupuncture The control group received oral administration of sodium valproate. This pharmaceutical medication is an anticonvulsant commonly used in the treatment of epilepsy, anorexia nervosa and bipolar disorder. Adverse affects associated with sodium valproate include fatigue, tremors, sedation and digestive disturbances. During pregnancy, this medication poses a very high risk for birth defects. Sodium valproate was administered twice daily with a dosage of 15-35 mg/kg for 30 days, comprising one course. The treatment lasted for three courses. The acupuncture group received needling in addition to the administration of sodium valproate. Scalp acupuncture needling was applied to the chest area, the epilepsy-control area and the chorea-tremor control area. Body style acupuncture was applied to Fengchi (GB 20), Baihui (DU 20), Sishencong (EX-HN1), Yintang (EX-HN3), Shuigou (DU 26), Neiguan (PC 6), Hegu (LI 4), Zusanli (ST 36), Fenglong (ST 40), Sanyinjiao (SP 6) and Taichong (LR 3). DU 26 is a vital acupoint in refreshing the brain. According to Traditional Chinese Medicine (TCM) principles, this acupuncture point clears the senses, calms the spirit and benefits the lumbar spine. DU 26 is indicated for both seizures and epilepsy. PC 6 is the Luo-connecting point of the Hand Jueyin channel. In TCM, PC 6 is used to calm the heart and spirit, regulate qi and suppress pain. PC 6 is indicated for the treatment of palpitations, chest pain, seizures and epilepsy, nausea, vomiting and heart beat issues. The lifting and thrusting needle technique was applied to DU 26, PC 6, EX-HN3, DU 20, EX-HN1 and LI 4. The reinforcing-reducing method was applied to other acupoints until the patient felt soreness and numbness consistent with the arrival of deqi. The needles were retained for 30 minutes and 10 days comprised one course of care. There was a 2 day break following each course. The treatment period was a total of 3 months. Following the completion of acupuncture therapy, a total of 12 acupuncture group patients showed no epilepsy related symptoms for at least 1 year. A total of 9 patients showed excellent improvements and 6 patients showed moderate improvements. The overall effective rate for the acupuncture group was 90.00% compared to 73.33% for the control group. Based on the positive clinical outcome, the research concludes that acupuncture combined with sodium valproate has a synergistic clinical effect leading to improved patient outcomes. AcuOffice TCM Theory Epilepsy is manifest in seizures, loss of consciousness, foaming of the mouth, headaches, dizziness, a stifling sensation in the chest, pallor, clenched jaw, incontinence of urine and feces, screams and/or staring of the eyes. According to TCM principles, epilepsy is an excess condition although it may arise from deficiencies in chronic cases. The onset of heredity related epilepsy is usually during early childhood. In TCM, epilepsy involves internal liver wind, liver qi stagnation and may also be exacerbated by dampness in the spleen and stomach, particularly due to irregular food intake. Fear and fright may trigger epilepsy. Fear disorders the qi and fright descends the qi thereby causing liver and kidney related internal wind due to deficiency. DU, REN, and Liver channel points are often selected for treatment during a seizure. The focus is to revive consciousness, dissolve phlegm, soothe the liver qi and to dispel the wind. Heart, Spleen and Kidney channel points are commonly selected following a seizure. The treatment principle is to soothe the spirit, nourish the heart and kidneys and to strengthen the spleen and stomach.
Reference: Niu, Xuexia. “Clinical observation on treating 30 cases of epilepsy by head and body acupuncture.” Clinical Journal of Chinese Medicine 6.4 (2014): 65-67. – See more at: http://www.healthcmi.com/Acupuncture-Continuing-Education-News/1306-acupuncture-synergizes-epilepsy-relief-new-finding#sthash.YvWIJEvh.dpuf
Blue Valley Acupuncture Clinic- Located in Dayton, WA.
DENISE LANE, EAMP, LAc; provides acupuncture treatments to folks in the greater Walla Walla Valley, Wa., Dayton and nearby towns.
Acupuncture Helps Depression Study Suggests
BLUE VALLEY ACUPUNCTURE CLINIC
SERVING GREATER WALLA WALLA, Washington, DAYTON AND NEARBY TOWNS
*article contributed by HealthCMI-Educational Classes for Acupuncturists and Nurses
Researchers conclude that ear acupuncture effectively reduces anxiety. The research team initiated the new investigation based on prior studies demonstrating that ear acupuncture reduces anxiety prior to dental treatments, surgery and during ambulance transport. Ear PointsThe research team discovered that ear acupuncture exerts “a specific and measurable effect” on anxiety levels.
Ear acupuncture, formally referred to as auricular acupuncture by licensed acupuncturists, involves using either standard filiform acupuncture needles or special auricular acupuncture needles. In this sham controlled trial, auricular acupuncture needles of 1.5mm length were inserted and retained for a total of 20 minutes and then removed. Sham needles were applied to patients in the control group. Looking at the photos below, one can see that the sham auricular needle does not have a penetrating tip. The needles are so tiny that they are affixed to the outer ear with an adhesive backing attached to each needle. In this study, Dongbang Acuprime brand auricular needles of a 0.22 diameter and 1.5mm length were used. Electroencephalography, a recording of brain electrical activity, was used to measure the depth of sedation.
Sham Ear Needle
The researchers documented both anti-anxiety and sedative effects of true ear acupuncture. Sham ear acupuncture did not produce a significant reduction in anxiety levels or induce a sedative effect. Electroencephalograph (EEG) measurements taken using the Bispectral Index System (BIS) confirmed the results. The sham versus true acupuncture results confirm that the placebo effect was not responsible for the therapeutic anti-anxiety effects of the auricular acupuncture. The researchers note, “When comparing the effects of real and sham needles, it was noted that there was a significantly higher reduction of
anxiety in the real-needles group” for both the NRS (Numeric Rating Scale) anxiety score and the STAI-Y (State-Trait Anxiety Inventory) score. BIS values “were significantly reduced during the real-needles application” at the10, 15 and 20 minute measuring points. The BIS (Bispectral Index System) encephalography device used in the study is depicted below.
Electroencephalograph
In related acupuncture continuing education research, investigators concluded that acupuncture relieves generalized anxiety disorder (GAD), a condition characterized by excessively intense and debilitating chronic anxiety. The researchers note that acupuncture has a fast effective action and high compliance. In addition, acupuncture has a relatively minimal risk of side effects compared with drug therapy. The acupuncture points in this study were located on the ankle and forearm at acupoints KI6 and LU7.
Many studies focus on the ability of acupuncture to reduce anxiety for specific conditions or situations. One recent study concludes that acupuncture reduces anxiety in women undergoing IVF (in vitro fertilization). A randomized-controlled study of 43 women undergoing IVF measured changes in anxiety levels. A total of four acupuncture treatments over a period of four weeks at a rate of once per week were administered. The acupuncture group received acupuncture at acupoints Yintang, HT7 (Shenmen), PC6 (Neiguan), CV17 (Shanzhong) and DU20 (Baihui). The control group received needle stimulation at non-acupuncture points near the areas of the true acupuncture points (sham acupuncture). The true acupuncture group showed a significant reduction in anxiety while the sham acupuncture group did not. The researchers concluded that acupuncture reduces anxiety and psychological strain for women undergoing IVF.
Another recent study receiving a great deal of attention is one that demonstrates that acupuncture reduces anxiety over dental procedures. In a patient-blinded randomized controlled investigation, researchers compared 182 patients. One group received true acupuncture at auricular points. The second group received sham acupuncture and a third group did not receive acupuncture or any medical procedures for the treatment of anxiety. The researchers measured anxiety levels prior to getting acupuncture and 20 minutes after receiving acupuncture, which was immediately prior to the administration of dental work. Anxiety levels in the true acupuncture group reduced significantly and but only very slightly in the sham acupuncture group. In the non-intervention group, anxiety increased. The researchers concluded that auricular acupuncture is both minimally invasive and “effectively reduces state anxiety before dental treatment.”
Researchers conducted another double-blinded study and concluded that both auricular acupuncture and body acupuncture are effective in reducing pre and post-operative anxiety. Pre and post-perative anxiety has been identified in approximately 80 percent of patients, which prompted this investigation. The ear acupuncture group received needle stimulation at point ear Shenmen. The body acupuncture group received acupuncture needle stimulation at Du20, Si Shen Cong, Yin Tang, LV3 and ST36. The needles were 0.25-.30mm in diameter and ranged between 25-40mm in length. Needle depth ranged from 0.2cm to 0.5cm. Acupuncture therapy was administered for a period of four weeks at two sessions per week for a total of eight acupuncture treatments. The Traditional Chinese Medicine (TCM) treatment principles were to increase lucidity, tranquilize by nourishing the Heart, calm the nerves and regulate the Qi. Both ear and body style acupuncture were effective in significantly reducing anxiety.
References:
Gagliardi, Giuseppe, Mariarosa Meneghetti, Francesco Ceccherelli, Andrea Giommi, and Marco Romoli. “Auricular Acupuncture for Anxiety in Health Care Volunteers: Randomized Crossover Study Comparing Real and Sham Needles.” Medical Acupuncture (2014).
Observation on the mechanism of acupuncture treatment for generalized anxiety disorder using Lieque (LU7), Zhaohai (KI6) as the main acupoints. Lin, Chuhua; Zhao, Xiaoyan; Liu, Xing; Fu, Wenbin. Bioinformatics and Biomedicine (BIBM), 2013 IEEE International Conference on. 18-21, 12-2-13
Effect of acupuncture on symptoms of anxiety in women undergoing in vitro fertilisation: a prospective randomised controlled study. Daniela Isoyama, Emerson Barchi Cordts, Angela Mara Bentes de Souza van Niewegen, Waldemar de Almeida Pereira de Carvalho, Simone Tiemi Matsumura, Caio Parente Barbosa. Acupunct Med acupmed-2011-010064Published Online First: 12 April 2012 doi:10.1136/acupmed-2011-01006.
Michalek-Sauberer, Andrea, Gusenleitner, Erich Gleiss, Andreas, Tepper, Gabor, Deusch, Engelbert. Auricular acupuncture effectively reduces state anxiety before dental treatment—a randomised controlled trial. Clinical Oral Investigations. Springer Berlin / Heidelberg; Issn: 1432-6981, 1-6.
Shengjun Wu, Jie Liang, Xia Zhu, Xufeng Liu, Danmin Miao. “Comparing the treatment effectiveness of body acupuncture and auricular acupuncture in preoperative anxiety treatment.” JRMS 2010; 16(1): 39-42.
– See more at: http://www.healthcmi.com/Acupuncture-Continuing-Education-News/1298-ear-acupuncture-sedates-anxiety-new-study#sthash.3fuKGvAf.dpuf
Acupuncture Study Brings Hope For Parkinson’s Disease Patients
By Brenda Duran, Senior Associate Editor

For people living with Parkinson’s disease, the future is full of obstacles and uncertainty.
This is the sole reason the second most prevalent neuro-degenerative disease that affects about 1 million people in the U.S., and 5 million worldwide has researchers constantly on the hunt for not only a cure, but also a way to improve the quality of life for patients.
By the year 2013, a current research study involving acupuncture is hoping to find answers for Parkinson’s disease patients living with one of the most debilitating side effects – fatigue.![]()
The research study funded by the Michael J. Fox Foundation for Parkinson’s Research is currently determining whether alternative Eastern medicine, specifically acupuncture, can help alleviate symptoms of severe fatigue in those living with Parkinson’s.
The foundation, which was established in 2000 by actor Michael J. Fox, is the largest funder of Parkinson’s research in the world. The organization has funded over $270 million in targeted Parkinson’s research to date including the latest study on acupuncture.
Dr. Benzi Kluger, assistant professor of neurology and psychiatry at the University of Colorado Hospital has been leading the study, which began in November 2010. The study is being conducted as a double-blind study to find whether acupuncture has a significant effect on Parkinson’s patients living with fatigue in their daily lives.
“Western medicine does not have good treatment for fatigue,” said Kluger. “Fatigue for patients with Parkinson’s is really different, it doesn’t improve with rest and is very disabling.”
 Fatigue affects approximately half of all Parkinson’s disease patients. Many of them do not get relief from medication and research has now focused on ancient Eastern medicine such as acupuncture to find answers, said Kluger.
Fatigue affects approximately half of all Parkinson’s disease patients. Many of them do not get relief from medication and research has now focused on ancient Eastern medicine such as acupuncture to find answers, said Kluger.
“We wanted to see if we can come up with alternative strategies that can also later help people with other neurological disorders in the future,” said Kluger.
Kluger approached the Parkinson’s foundation with his study because he said he was interested in non-motor systems in Parkinson’s patients. Non-motor symptoms are the most common symptoms that develop first in patients and one of them is fatigue.
Jamie Eberling, associate director of research programs at the Michael J. Fox Foundation for Parkinson’s Research said Kluger’s study was chosen based on its merits and because it was something of interest to their donor base.
“We are always interested in different types of approaches,” said Eberling. “We are always open to new things, we wish we could see more of these types of studies being presented.”
The foundation in the past has funded studies on exercise and even singing for speech problems as well as dancing for motor impairment in Parkinson’s disease patients. They review 800 grant proposals a year and are currently supporting more than 300 research projects in industry, academia and government.
Kluger’s acupuncture study has a total of 22 patients participating right now. The goal is to have 90-100 patients by the study’s end date in 2013.
Patients who joined the study initially came in for a screening visit and filled out a questionnaire about fatigue and their beliefs about acupuncture and alternative medicine. Once people were screened into the study, they were randomized with twice weekly sham or real acupuncture.
Patients in the study are blindfolded while they are receiving acupuncture treatment and Kluger said he doesn’t know which patients are receiving acupuncture treatment and which patients are receiving placebo.
Three acupuncturists have been working on the study subjects placing needles in acupuncture points on the patient’s face and back. For patients who are in the placebo group, the acupuncturists may place non-penetrating needles in spots that aren’t typical acupuncture spots.
Kluger said in the spring, his team is going to try to shell out a paper on the sham acupuncture after spending a lot of time learning how to remove the sham needles to create a really good placebo procedure.
So far, Kluger said he has seen dramatic improvement in fatigue in some of the study subjects. “People have gone back to doing activities that they haven’t done in years,” he said. Since the statistical data is not yet completed, Kluger said he wouldn’t know which group has benefitted the most.
Kluger noted that a large majority of Parkinson’s disease patients already use a form of alternative medicine – acupuncture, massage, herbs and chiropractic care, but until now, there weren’t many evidence-based studies to determine whether acupuncture is effective for symptoms such as fatigue.
The neuro-degenerative disease affects between 1 percent and 2 percent of people over the age of 65. Those diagnosed with the disease will lose neurons in specific parts of the brain, affecting muscle movement and control over time.
Kluger said if he finds that acupuncture can be used as an alternative form of medicine to alleviate the symptoms of severe fatigue, it might help insurance companies extend their coverage of the treatment.
“We will also be able to see if acupuncture would be effective for people with other diseases like cancer and MS (Multiple Sclerosis),” Kluger said.
Focusing most of his medical career in Western medicine, Kluger said he has really enjoyed doing research on Eastern medicine and finding out about the potential it has to heal people.
“For me it has been a wonderful opportunity to work with acupuncturists to really start to delve into acupuncture. One of my goals is to come out of it with an open mind,” he said. “It’s been really fun to explore alternative ways to help these patients. We are hopeful.”
If you would like to know more about the study contact etta.abaca@ucdenver.edu or call 303-724-2193.







